ARDMS AB-Abdomen Exam Questions
- Topic 1: Anatomy, Perfusion, and Function: This section of the exam measures the skills of abdominal sonographers and focuses on evaluating the physical characteristics, blood flow, and overall function of abdominal structures. Candidates must understand how to assess organs such as the liver, kidneys, pancreas, and spleen for size, shape, and movement. It also involves analyzing perfusion to determine how effectively blood circulates through these organs. The goal is to ensure accurate interpretation of both normal and abnormal functions within the abdominal cavity using sonographic imaging.
- Topic 2: Pathology, Vascular Abnormalities, Trauma, and Postoperative Anatomy: This section of the exam evaluates the abilities of diagnostic medical sonographers and covers the detection and analysis of diseases, vascular issues, trauma-related damage, and surgical alterations in abdominal anatomy. Candidates are expected to identify abnormal growths, inflammations, obstructions, or vascular irregularities that may affect abdominal organs. They must also recognize post-surgical changes and assess healing or complications through imaging. The emphasis is on correlating pathological findings with clinical data to produce precise diagnostic reports that guide further medical management.
- Topic 3: Abdominal Physics: This section of the exam measures the knowledge of ultrasound technicians in applying imaging physics principles to abdominal sonography. It includes understanding how to optimize ultrasound equipment settings for the best image quality and how to identify and correct imaging artifacts that can distort interpretation. Candidates should demonstrate technical proficiency in handling transducers, adjusting frequency, and managing depth and gain to obtain clear, diagnostic-quality images while minimizing errors caused by acoustic artifacts.
- Topic 4: Clinical Care, Practice, and Quality Assurance: This section of the exam tests the competencies of clinical ultrasound specialists and focuses on integrating patient care standards, clinical data, and procedural accuracy in abdominal imaging. It assesses the candidate ability to follow established medical guidelines, ensure correct measurements, and provide assistance during interventional or diagnostic procedures. Additionally, this domain emphasizes maintaining high-quality imaging practices and ensuring patient safety. Effective communication, adherence to protocols, and continuous quality improvement are key aspects of this section.
Free ARDMS AB-Abdomen Exam Actual Questions
Note: Premium Questions for AB-Abdomen were last updated On May. 29, 2026 (see below)
What is the most common ultrasound appearance of the pancreas in mild acute pancreatitis?
In mild acute pancreatitis, the pancreas often appears diffusely enlarged and slightly hypoechoic due to edema and inflammation. However, in very early or mild cases, the pancreas may still appear normal. Heterogeneous echotexture may develop in more severe or necrotizing pancreatitis.
According to Rumack's Diagnostic Ultrasound:
''In mild pancreatitis, the pancreas is commonly enlarged and hypoechoic due to inflammatory edema.''
Rumack CM, Wilson SR, Charboneau JW, Levine D. Diagnostic Ultrasound. 5th ed. Elsevier, 2017.
AIUM Practice Parameter for the Performance of an Ultrasound Examination of the Abdomen, 2020.
---
Which type of artifact is indicated by the arrows on this image?
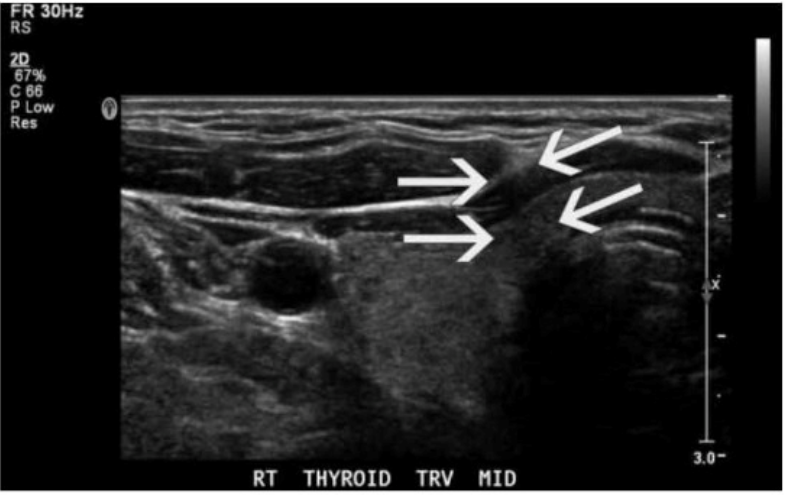
The ultrasound image of the thyroid clearly shows posterior shadowing originating from the lateral edges of a rounded structure, which is indicative of edge shadow artifact. Edge shadowing occurs when an ultrasound beam passes tangentially to a rounded or curved structure, such as a cyst or blood vessel. The difference in sound wave refraction and beam divergence at the edges leads to decreased echo signals deep to the edges, creating linear hypoechoic bands --- which is exactly what the arrows are pointing to in the image.
Edge shadow artifact is purely a result of beam physics and not a real anatomic or pathologic finding.
Key characteristics of edge shadowing:
Appears as a narrow, linear hypoechoic (dark) shadow extending deep to the edge of a curved interface (e.g., cyst, vessel, thyroid nodule)
Caused by refraction and beam deflection, leading to reduced beam intensity distal to the edges
Most commonly seen adjacent to cysts or fluid-filled structures
Differentiation from other options:
A . Focal enhancement: Appears as increased echogenicity distal to a fluid-filled structure due to lower attenuation of the sound beam through fluid (opposite of shadowing).
C . Speed error: A less common artifact that results in displacement of structures due to variation in assumed sound speed.
D . Comet tail: A reverberation artifact that appears as a series of closely spaced bright echoes, often associated with metallic objects or cholesterol crystals in adenomyomatosis.
Rumack CM, Wilson SR, Charboneau JW, Levine D. Diagnostic Ultrasound. 5th Edition. Elsevier, 2018. Chapter: Ultrasound Physics and Artifacts, pp. 38--42.
Kremkau FW. Sonography Principles and Instruments. 9th Edition. Elsevier, 2015. Chapter: Image Artifacts, pp. 132--136.
Which sonographic finding is associated with normal postprocedural Doppler of a transjugular intrahepatic portosystemic shunt (TIPS)?
After successful TIPS placement, the intrahepatic portal venous branches continue to exhibit hepatopetal (toward the liver) flow, while the stent itself shows continuous, relatively high-velocity monophasic flow. Hepatofugal flow in intrahepatic branches may indicate shunt dysfunction.
According to Zwiebel's Introduction to Vascular Ultrasound:
''Normal post-TIPS Doppler shows hepatopetal flow in the intrahepatic portal veins and continuous high-velocity flow within the stent.''
Zwiebel WJ, Pellerito JS. Introduction to Vascular Ultrasound. 6th ed. Elsevier, 2019.
AIUM Practice Parameter for the Performance of Portal Venous Ultrasound, 2020.
---
Which technique is best for demonstrating the characteristic of the small hepatic lesion identified by the arrow on this image?
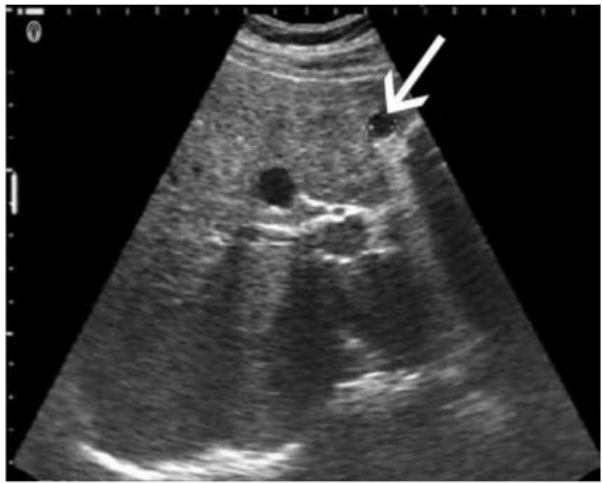
The image shows a small hepatic lesion located very close to the anterior liver capsule, as indicated by the arrow. When imaging very superficial or near-field structures like subcapsular hepatic lesions, using a standoff pad is the most effective technique for optimizing visualization.
A standoff pad (also known as an acoustic stand-off or gel pad) helps increase the distance between the transducer and the superficial target. This improves the focus and beam shape for near-field imaging and minimizes reverberation and ring-down artifacts. It allows better evaluation of superficial lesions by positioning them within the focal zone of the transducer, which is usually set a few millimeters below the probe surface.
Differentiation from other options:
A . Decrease depth: While reducing depth can help center deeper lesions in the field of view, it does not address issues with near-field resolution.
B . Scan in upright position: This may help in gallbladder or fluid positioning but is not optimal for improving visualization of superficial liver lesions.
C . Move the transducer focus: Adjusting focus deeper into the image won't enhance resolution of very superficial structures unless a standoff is used to bring the lesion into the focal zone.
Rumack CM, Wilson SR, Charboneau JW, Levine D. Diagnostic Ultrasound. 5th Edition. Elsevier, 2018. Chapter: Liver, pp. 80--84.
Kremkau FW. Sonography: Principles and Instruments. 9th Edition. Elsevier, 2015. Chapter: Image Formation and Optimization, pp. 114--117.
AIUM Practice Parameter for the Performance of an Ultrasound Examination of the Abdomen and/or Retroperitoneum, 2020.
Which congenital disorder is most consistent with the finding identified by the arrow on this image?
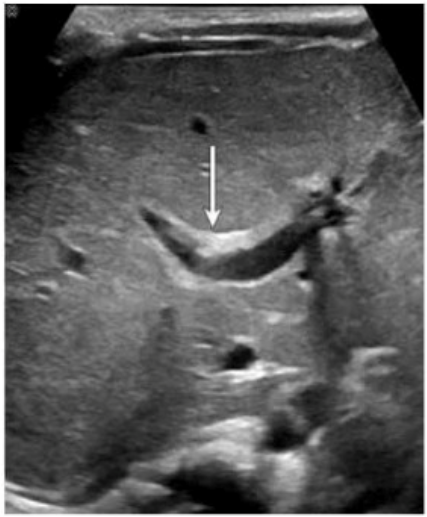
The image demonstrates a characteristic 'central dot sign' --- a hallmark finding of Caroli disease. This is best appreciated on ultrasound as a cystic dilation of the intrahepatic bile ducts with a central echogenic dot or linear structure (which corresponds to the portal vein and fibrous tissue within the dilated duct). The arrow in the image points to one such dilated duct.
Caroli disease is a rare congenital disorder characterized by segmental, saccular dilation of intrahepatic bile ducts. It is often associated with congenital hepatic fibrosis and may predispose to cholangitis, stone formation, and even cholangiocarcinoma.
Key ultrasound features of Caroli disease:
Cystic or saccular dilations of the intrahepatic bile ducts
The 'central dot sign' --- echogenic focus in the center of the dilated ducts (representing portal vein radicle or fibrous tissue)
May show associated hepatosplenomegaly or signs of portal hypertension
Differentiation from other options:
A . Sclerosing cholangitis: Typically causes diffuse or segmental biliary ductal wall thickening and stricturing; does not present with cystic dilations.
B . Alagille syndrome: A multisystem disorder often characterized by a paucity of intrahepatic bile ducts, not dilation.
D . Biliary atresia: Presents in infancy with obliteration of extrahepatic bile ducts, echogenic 'triangular cord' sign, and absence of a visible gallbladder. It does not cause ductal dilation.
Rumack CM, Wilson SR, Charboneau JW, Levine D. Diagnostic Ultrasound. 5th Edition. Elsevier, 2018. Chapter: Biliary System, pp. 152--155.
Radiopaedia.org. Caroli disease. https://radiopaedia.org/articles/caroli-disease
American College of Radiology (ACR). ACR--SPR Practice Parameter for the Performance of Pediatric Abdominal Ultrasound, 2022.
- Select Question Types you want
- Set your Desired Pass Percentage
- Allocate Time (Hours : Minutes)
- Create Multiple Practice tests with Limited Questions
- Customer Support
Ashley Garcia
13 days agoJason Edwards
24 days agoJennifer Jackson
1 month agoJessica Nguyen
27 days agoJeffrey Young
1 month agoTimothy Reed
22 days agoMichelle Thomas
17 days agoHarold Baker
14 days agoSharika
2 months agoSteffanie
2 months agoNettie
2 months agoJohnathon
3 months agoStevie
3 months agoCarey
3 months agoYoko
3 months agoMable
4 months agoNathan
4 months agoTheron
4 months agoBrendan
4 months agoFranklyn
5 months agoKris
5 months agoBuffy
5 months agoMarcelle
5 months agoMattie
6 months agoCarin
6 months agoLeonora
6 months agoShaunna
6 months agoChuck
7 months agoJohna
7 months ago